Streeck Lab fired up about recent findings in Nature Medicine: HIV preferentially infects CD4 T cells and in particular those that recognize HIV.
 The primary role of CD4 T cells is to help other cells and orchestrate the different arms of the immune system. Their importance is best illustrated by how completely the immune response collapses after most of the CD4 T cells are destroyed. This stage of HIV infection is known as AIDS. Given their preferential infection and depletion, HIV-specific CD4 cells have not been a major focus of vaccine research. However, these cells may still have an important, unappreciated role in controlling HIV infection.
The primary role of CD4 T cells is to help other cells and orchestrate the different arms of the immune system. Their importance is best illustrated by how completely the immune response collapses after most of the CD4 T cells are destroyed. This stage of HIV infection is known as AIDS. Given their preferential infection and depletion, HIV-specific CD4 cells have not been a major focus of vaccine research. However, these cells may still have an important, unappreciated role in controlling HIV infection.
Published June 23rd (Advanced Online Publication) in Nature Medicine a team of researchers lead by Hendrik Streeck now demonstrate that HIV-specific CD4 T cells, despite their role as target cells, may play an important role in controlling viral loads. In a cohort of over 1000 chronically HIV infected individuals the authors show that certain HLA class II alleles are associated with HIV control, while others are associated with rather rapid disease progression. They also found that the HLA class II alleles that are associated with HIV control also restrict for a greater number of HIV-specific CD4 T cell responses, but bind those with lower functional avidity. In contrast, the HLA class II responses associated with rather unfavorable disease course restrict for less HIV-specific CD4 T cell responses but bind those with higher functional avidity. The Streeck lab now follows the hypothesis whether HLA-DRB1 variants linked with low viremia may bind at lower avidity and may show greater promiscuity in their peptide interactions as compared to those associated with high viremia. Given this strong association the Lab hypothesizes that HIV-specific CD4 T cell responses recognizing HIV peptides with high specificity and avidity reach a higher activation status and are therefore more susceptible to HIV infection or activation-induced cell death.
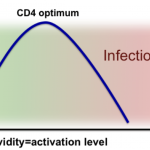
We suggest a model of an HIV-specific CD4 T cell activation optimum that allows CD4 T cells to provide sufficient helper function and/or antiviral activity but remain mostly preserved from activation-induced cell death and susceptibility to HIV infection (figure). Thus, the strength of interactions for HIV-specific CD4 T cell responses will not only determine the selective depletion of HIV-specific CD4 T cell responses, but also the immunodominance pattern of HIV-specific CD4 T cell responses and the further course of disease progression.
Read the full article here.
Association of HLA-DRB1–restricted CD4+ T cell responses with HIV immune control
Ranasinghe S, Cutler S, Davis I, Lu R, Soghoian DZ, Qi Y, Sidney J, Kranias G, Flanders MD, Lindqvist M, Kuhl B, Alter G, Deeks SG, Walker BD, Gao X, Sette A, Carrington M, Streeck H.
Abstract: The contribution of HLA class II–restricted CD4+ T cell responses to HIV immune control is poorly defined. Here, we delineated previously uncharacterized peptide-DRB1 restrictions in functional assays and analyzed the host genetic effects of HLA-DRB1 alleles on HIV viremia in a large cohort of HIV controllers and progressors. We found distinct stratifications in the effect of HLA-DRB1alleles on HIV viremia, with HLA-DRB1*15:02 significantly associated with low viremia and HLA-DRB1*03:01 significantly associated with high viremia. Notably, a subgroup of HLA-DRB1 variants linked with low viremia showed the ability to promiscuously present a larger breadth of peptides with lower functional avidity when compared to HLA-DRB1 variants linked with high viremia. Our data provide systematic evidence that HLA-DRB1 variant expression has a considerable impact on the control of HIV replication, an effect that seems to be mediated primarily by the protein specificity of CD4+ T cell responses to HIV Gag and Nef.
